Longer length GORE VIABAHN Endoprosthesis receives CE mark approval
Published date : 19 July 2010
Article date : 19 July 2010
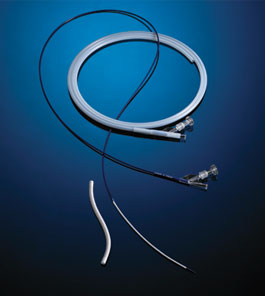 The GORE VIABAHN Endoprosthesis with PROPATEN Bioactive Surface has recently received CE mark approval. The new 25cm device is the longest length stent-graft available, designed to cover more of the lesion in the superficial femoral artery (SFA) potentially reducing the need for multiple devices.
The GORE VIABAHN Endoprosthesis with PROPATEN Bioactive Surface has recently received CE mark approval. The new 25cm device is the longest length stent-graft available, designed to cover more of the lesion in the superficial femoral artery (SFA) potentially reducing the need for multiple devices.
The device features a precision laser trimming technology used to remove excess material, resulting in a contoured proximal edge that may improve flow dynamics at the proximal end. Removal of excess material at the proximal edge improves device apposition to the vessel wall when oversizing prevents device expansion to its nominal diameter. The device also incorporates the PROPATEN Bioactive Surface which utilises end-point immobilisation of derivatised heparin to the endoprosthesis luminal surface. This proprietary surface technology preserves the heparin bioactive sites such that they remain free to interact with the blood at the device surface without being consumed. The original GORE HEMOBAHN Endoprosthesis was introduced to Europe in 1996; the GORE VIABAHN Endoprosthesis with PROPATEN Bioactive Surface was first approved for use in the EU in December 2008.
“In 1996, the [GORE] HEMOBAHN-VIABAHN device was the first SFA stent-graft that had good patency rates and it came already in 15cm length,” said Dr Jacques Bleyn, Antwerp Blood-Vessel Center, Antwerp, Belgium. “Because long SFA occlusions can be treated endovascularly with the GORE VIABAHN device, Gore took this best SFA device and made it better: heparin bonded and a new length of 25cm.”
The device is available with a low-profile delivery system that gives interventionalists a more streamlined approach to re-line the peripheral arteries. It is constructed with a durable, reinforced, biocompatible, ePTFE liner attached to an external nitinol stent structure. The excellent flexibility of the endoprosthesis enables it to better traverse tortuous areas of the SFA and conform more closely to the complex anatomy of the artery.


